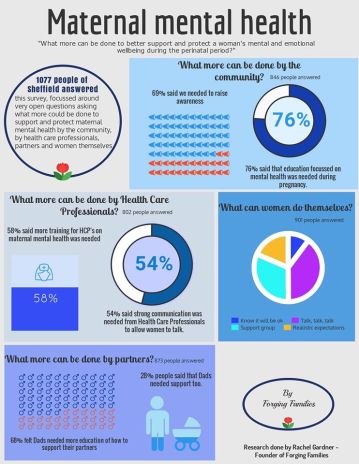
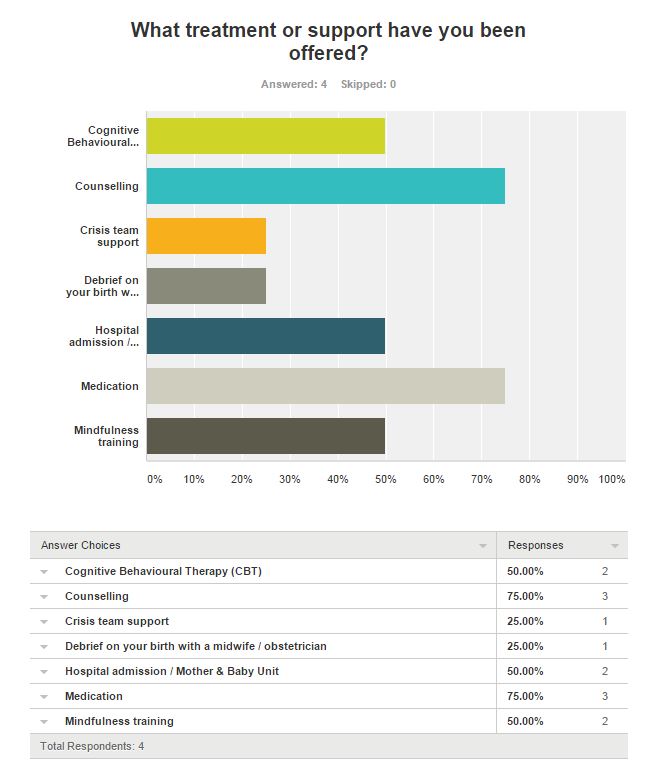
Before the National Maternity Review claimed everyone’s attention, we had The Lancet Breastfeeding Series which was big news in the infant feeding world. The WBTi team put together this wonderful Open Letter in response and many productive discussions were had.
Inevitably, social media being what it is, there were also unproductive discussions between people who found it hard to see each other’s point of view. I have discussed acknowledging each other’s truths before when I wrote about Infant Feeding for the #MatExp campaign, but what occurred to me this time around was that when we discuss these things we all have a different person in mind. We think that we’re discussing things in general terms, for the benefit of all readers or listeners, but in truth we are discussing our own experience, or the situation of a close friend or family member, and we are speaking to that person who annoyed us hugely at the coffee shop, or our parent who doesn’t support our feeding choices. This colours a great deal of our discussion and goes some way to explain why emotions can run high. There are real people behind the generalisations, real experiences, and sometimes real pain.
So I thought I would take a leaf out of the #MatExp book and try to gather some differing voices. This blog post is a snapshot of feeding experiences, it would take a far wider study to truly hear “all voices” in this regard. But I hope I can present some alternative people, so that the next time we all come together to discuss feeding choices we can perhaps bear in mind the experiences of people different from us. Stepping into other people’s shoes can help to bring us together.
*****************************
Lucy – “I feel good that he’s alive and thriving”

Lucy chose to breastfeed her baby, as most women do, but had to switch to formula at 5 days old when baby was admitted to special care with 16% weight loss and severe jaundice. “I had no positive support at all on the maternity ward or at home from feeding support workers. No one picked up on the fact that my son wasn’t latching on at all and one midwife squeezed my nipple into his mouth – it was very painful. I had no support for formula feeding at all either, apart from the nurses in special care who were amazing in helping us get to grips with bottle feeding. Most of my information about my feeding choice came from them.”
How did friends and family support your feeding choices? “My husband and mum were amazing, but my brothers and sisters-in-law didn’t really understand why I wasn’t breastfeeding. My brother would make constant comments like ‘bottle fed babies throw up more’ and ‘bottle fed babies are much easier’. My mum didn’t really understand the importance of sterilising.”
“I had one mother come up to me at a family centre as I was preparing a bottle when my son was a couple of months old and she told me ‘It’s a shame you’re not breastfeeding as that’s best for baby’. To which I replied that I preferred an alive baby to a dead one. I feel bad about my feeding choice most of the time. I feel less guilty now though as he’s thrived so much. I do feel like I’ve let him down but I feel good that he’s alive and thriving.”
Liz and Alan – “happy that the grandchildren are happy and fed”

Liz and Alan’s daughter Sarah breastfed her eldest son for about six weeks before switching to formula. She then breastfed her middle son exclusively for ten months, and is four months into breastfeeding her youngest.
Liz breastfed Sarah for 10 months “which was full term for her, she decided she didn’t want it so just stopped herself. My son who was a very small baby had trouble latching so after three weeks of breastfeeding I switched to formula. The midwives helped me with both of my children. They were on hand to answer questions and were supportive of my choices with regard to feeding. I had a special care midwife for my son because he was premature and so small (5lb) and she was great.”
Liz is pleased that Sarah is able to breastfeed “but I was also supportive when she decided to switch to formula with her first child. I fully support Sarah however she chooses to feed.” Liz explained that she had not seen any infant feeding information aimed at grandparents, but that “I personally don’t feel the need for it as I know the benefits having breastfed and formula fed my own, so I know the pros and cons. I am happy that the children are happy and fed.”
Liz did feel that it could be useful for there to be information available to grandparents about expressing breastmilk, the importance of sterilising bottles and so on with regard to looking after the grandchildren whilst their parents are at work.
Alan feels that it is great that Sarah is breastfeeding her son as “it’s the natural way to do it.” He feels that the way his daughter has fed the grandchildren gives them the best, and he has no concerns whatsoever. When it comes to infant feeding information for grandparents, he also commented that perhaps “grandparents who look after young children (as childcare for working parents) might like up to date information about how best to feed them.”
Sarah said of her parents “I feel very blessed to have them, they support me completely and would no matter how I chose to feed.”
Sarah-Jane – “it was the norm in my family, it was what I wanted to do”

Sarah-Jane breastfed her daughter until she was twelve months old. “From the moment I found out I was pregnant I wanted to breastfeed. It was the norm in my family, my mother breastfed me, my sister breastfed, it was what I wanted to do. I also researched the benefits of breastfeeding which confirmed that I was making the right choice for me and my family. As I returned to work when my daughter was nearly ten months old I would express each day at work to ensure she had enough milk for her time at the childminder’s. This worked well for us and she was happy to take a bottle of expressed milk when I was not around.
I know I was extremely lucky in that my midwife was very pro breastfeeding and was very knowledgeable about it. She prepared me for all scenarios on what to expect, what I can do and linked me into the local breastfeeding groups. Following this my health visitor was also a massive support in my decision to continue to breastfeed beyond six months – she enabled me to feel confident in the choice I was making and gave me information to assist me in this choice. My local breastfeeding support group was also led by health visitors which was fantastic – meeting like-minded mums, being able to discuss things with people who were going through exactly what I was was a great support to me.
My husband was amazing, he supported me from the beginning with my decision to breastfeed our child, so were my family. For me I think it would have been weird if I hadn’t have breastfed as it was just assumed that I would. I was never made to feel uncomfortable, I was always encouraged to feed wherever I needed to. My friends were also supportive and accepting of the choice I had made. I have made some long term friends from my breastfeeding support group.
I got most of my information on infant feeding from Internet research and my family, in terms of finding the information in the lead up to having my baby. I had seen my sister feed her two babies so I knew some of what to expect. As my due date got closer I did use my appointments with my midwife to seek further information and discuss my concerns.
I feel good about my feeding choice knowing I was giving my baby the best start in life I could, also the bond I have with my little girl is so worthwhile. When you’re feeding your baby and they gaze up at you in that moment I know and still know now that I did the best for her, this makes me feel good.
Lisa – “my friends and family were in awe of me”

Lisa wanted to breastfeed exclusively but her baby has feeding issues – a tongue tie, reflux and a milk allergy, so she was combi-fed.
“I breastfed in the house and expressed or gave formula – I could only feed indoors as it would take my baby hours to take a feed due to reflux. I went to breastfeeding support groups but I found that as my baby got more unsettled due to milk allergy and reflux that I couldn’t really get the support I required. My daughter didn’t respond much to any technique and advice.
My friends and family were great, they in fact said they were in awe of me as they know how difficult it has been, but I couldn’t really have much support from them as they hadn’t been in the same position. Healthcare professionals just pushed my daughter on my breast which obviously made her scream. Often at times I felt that they thought I was just a new mum that couldn’t cope.
Some friends and family members told me it didn’t matter that my baby had formula as well as breastmilk. I know they were trying to be helpful and meant well, but I didn’t find it helped at all. I got myself really stressed and people would tell me not to be silly, but I felt it was a big deal to me.
I have got most of my information on my feeding choice from online support.
I felt bad when I was still breastfeeding and I had to give my daughter a bottle of prescription milk. I had to cut other stuff from my diet which I found extremely difficult. Being a tired new mum with a high needs baby was difficult enough.
I have nothing against women that choose to formula feed, but I wanted to exclusively breastfeed and I felt a failure that I couldn’t. But despite my baby’s issues she has still continued to put on weight and is otherwise healthy and this makes me feel good.
Liam – “it’s natural, relaxing and peaceful”

Liam’s partner Gill has breastfed their two children to natural term. Liam is very happy about this as he can see how happy it makes his children. “Knowing that it is best for them makes me positive about it. Natural, relaxing and peaceful. It works for Gill because she buys into the reasons for doing it so is very keen to continue. We don’t have to use any false breastmilk replacements which cuts costs, reduces environmental stress – it takes less thinking. With William it was a learning curve so it is easier these days for Hattie. I’ve learnt to understand how I can help and fit into the approach.
A few people asked questions when both Hattie and William were younger about how Gill had to be there for them most of the time – when would Gill get any time away? But people have made positive or neutral comments on the whole.
I don’t have any other vision in mind of how this should all work, i.e. non breastfeeding, so nothing to compare it to. I think it’s sad that so many children miss out – including myself. Breastfeeding is very good at calming children – when managing William and Hattie at times on my own I don’t have this to depend on, so sometimes I feel a little lost when it’s not available.
I remember reading about the positives of breastfeeding for mum and baby, and the support that is needed. I recall the good midwives showing Gill and me how to approach it, techniques and things to do. I listened to Gill about what things she needed, and I wasn’t influenced by anyone who was negative about it.”
Gill recalls that “a different midwife came to the house every day for the first eight days post birth ‘just’ to help with breastfeeding. I was at the point of giving up numerous times, at the time I resented Liam for his resolute determination that we would continue to breastfeed. He was SO encouraging I could have killed him. But I am so very grateful now.”
Sarah – “everyone pitches in and helps, no one judges”

“I formula fed Joe from day one, mainly because of the experience I had with my eldest. I felt like I wasn’t ready to try breastfeeding again.
I didn’t have any advice or help from any health visitors or midwives. I think because I was so confident in my decision they didn’t feel I needed any. Luckily my family are all pretty chilled. They would have helped no matter what my choice was. My mum even took a week off after my other half went back to work just in case.
When I said I didn’t want to breastfeed I wish someone had asked why and had explained my experience with Grace to me. As mad as it sounds, I had no idea that I would struggle with my milk supply with Grace after losing so much blood and having a traumatic birth. If we’d have talked that through I would have felt better. It was only from an online forum that I knew with hindsight what had happened.
I get most of my infant feeding information from the World Health Organisation and NHS websites.
I can honestly say that all of my friends and family have been helpful. Everyone pitches in and helps, no one judges. But when Joe was a few days old I went to a coffee shop with Grace and my mum. A lady in her late fifties walked past me and said “breast really is best you know dear”!
I constantly feel bad about my choice because I didn’t even try. I know now that my experience with Grace was not my fault, and I had poor advice from horrible midwives. I worry I have deprived Joe and I’ve not provided myself with the benefits of breastfeeding either. But I feel good because we have an amazing bond. He is thriving and my other half was able to help with the nights in the early days.”
Julie – “I chose to breastfeed to natural term because why would I stop?”

“I breastfed both my children: my first son until he was 3 years and 9 months when he naturally weaned and my younger son, who is currently 3 years and 3 months, is “still” breastfeeding. I breastfed throughout pregnancy and tandem fed both boys for around one year.
I chose to breastfeed because it is natural and normal. I chose not to formula feed because of the dangers associated with doing so. I chose to breastfeed to natural term because why would I stop? The benefits of breastfeeding do not decrease with the age of the child. Through breastfeeding I have provided nutrition and protection to my children, it has been a comforter and soother, it has helped them calm down after tantrums, it has helped them sleep and it is the single most important thing I have done for both my children.
The healthcare professionals I have been in contact with were generally supportive of my choice, but did not provide me with any useful or practical advice. I received basic help from the midwives in hospital after the birth of my first child and then received some advice from a breastfeeding support worker, when after a few days I panicked that my milk had not come in. When my second child was born the midwife was delighted that I was also breastfeeding my then 2 year old as she had fed all four of her children to natural term. She was extremely helpful in reminding me of the difference between feeding a newborn and the more experienced toddler.
Sadly I have received inaccurate advice (going against the WHO code) and even personal opinion from healthcare professionals about both breastfeeding and natural term breastfeeding. I have been told that breastmilk causes tooth decay, that there is no benefit after six months and that I am making a rod for my own back by feeding to sleep – all of which is inaccurate. When my second son was born, I took both children to a breastfeeding support group in Lichfield. The other mums were very welcoming and supportive, and asked my advice as an experienced breastfeeding mummy. The health professional however said that I would make a mockery of her statistics with a child breastfeeding at nearly 3 years old. Another healthcare professional used to scoff at me for breastfeeding and said to me that formula didn’t do her children any harm.
I feel sorry for women who receive this advice and hear these comments and believe it.
My husband has always been very supportive. He is very helpful in providing refreshments whilst I am breastfeeding, as well as staying awake at night to chat to me. Our families and friends have been accepting, even though they may not agree with my choice to breastfeed to natural term. I have met dozens of women who have breastfed their children for up to six and seven years, and they have been especially supportive of me. Many of these have become good friends.
I have occasionally had comments about when I will stop breastfeeding from friends. I choose not to be embarrassed and have continued to feed on demand irrespective of my child’s age. I have never had any negative comments. I have had many people congratulating me and offering me admiration for feeding my boys to natural term. Many people have expressed their regret in giving up breastfeeding.
I get the majority of my infant feeding information from the Association of Breastfeeding Mothers and La Leche League.
I am very proud that I have given my boys the best start in life.”
Laura – “I am able to make anything that upsets them instantly better”

“I set out to exclusively breastfeed because I had some general understanding of the risks associated with not breastfeeding and I didn’t want to expose my babies to them. I ended up supplementing my first baby with expressed milk and formula top up until around 13 weeks and then managed to return to exclusive breastfeeding. My second baby has been exclusively breastfed.
I received no support from healthcare professionals with my first baby. A support worker at the hospital helped me for about half an hour. The midwives there were genuinely too busy to help me. They tried but were called away within a couple of minutes every time they sat down.
The community midwives were unpleasant, treated me like an inconvenience they didn’t have time for and strongly pressured me to formula feed. I gave into this pressure, even though it felt so wrong, because I didn’t know where else to turn for help. I thought they would help me, not undermine me. I didn’t have the strength to fight them.
I now realise they simply didn’t have the knowledge to support me. I wish they’d been honest and directed me to some properly qualified support, instead of covering their backs by telling me I was endangering my baby by persisting with exclusively breastfeeding. I now know she has a (fairly obvious) tongue tie but they never got close enough to check and I’ll never know if that was the problem.
My husband was (and is) wonderful. He took over everything in our lives so that I only had to express milk and feed our daughter. He constantly reminded me that he was on board with whatever I chose to do and told me he was proud or me. My mum knew nothing about breastfeeding but would drop in, make me a cuppa, do the dishes, stick some laundry on and then leave us to it. So, so helpful. Other people who visited stayed for hours, made a mess and helped very little with practical things. Normally I could handle that but whilst trying to recover exclusive breastfeeding it nearly tipped me over the edge.
Back then I got most of my infant feeding information from the Kellymom website and Mumsnet. Nowadays it’s La Leche League’s The Womanly Art of Breastfeeding, and still Kellymom but also Dr Jack Newman’s site.
My Mum regularly says she thinks it’s great that I have breastfed the kids but….. A woman on a train once said ‘It’s so lovely to see a baby being fed properly. That’ll be why he’s such a happy little chap.’ I feel good about my feeding choice because it means I am able to make pretty much anything that upsets them better instantly. Also, knowing I’ve done my best for them, which is the least they deserve from me.”
Ruth – “a healthy mum means a mum who could care for her child”

I began breastfeeding my second child because I had breastfed my first child as I wanted to give my babies the natural milk, and believe it should be the default position. But two things intervened that meant I formula fed him. The first of these was a tongue tie that I didn’t get support with until he was 3 ½ months old, and even then it was my own vigilance and questioning and then my own research and seeking a private appointment which resolved it. This is something that might have threatened my ability to breastfeed in any case. However, within a week of his birth I was diagnosed with postpartum psychosis and put on medication that I was told was not compatible with feeding, and I was so knocked out by the medication others had to be with my baby at night. In the end he was formula fed long term.
In the hospital the midwives kept checking his latch but could find nothing wrong so they lacked the experience to question whether tongue tie had some bearing on it. Once at home he was having some formula and the midwife gave me some support on how much to make up and some basic info on formula feeding a newborn, since I had breastfed my first child. There was no support for reinstating breastfeeds or checking the latch or for further problems. But I also managed to do some feeds as breastfeeds especially as my milk came in and the pain subsided a little. Then when the psychosis took hold the midwife ensured I got a diagnosis but once the mental health team took over the support was for me and not really my feeding choices.
I could have done with some support about the logistics of fully formula feeding. One of the female mental health nurses just shared her own anecdotal information to help me get my head around it but it wasn’t correct info on making up bottles safely. Their advice was for me not to breastfeed whilst taking quetiapine and diazepam. I do not know if this is accurate. However it has to be said that as I wasn’t able to do the nights as I was knocked out by the meds, I would have had to have combi-fed at the very least, but I could have had some support for this maybe. I am still unclear to this day whether or not my medications are compatible with feeding so I would think that accurate info on drugs and breastfeeding needs to be more readily available to health professionals.
As I moved on to formula the midwife stopped me to say that formula feeding would be a lot harder as if you had an unsettled baby and couldn’t work out if he needed feeding or not then you couldn’t just whip a breast out and see. You would have to make up a bottle and risk wasting it. It made me very anxious about bottle feeding which didn’t help my mental state.
My husband and family and friends were all supportive and realised it was something that had to be so, due to the postpartum psychosis, and I received no criticism.
My information about formula feeding came from the midwife who gave me information by answering some questions, and then I looked back at a book that the NHS issued with my first son of caring for baby and the info about formula was there. And a friend who formula fed her second helped me out with information, from what bottles to buy to tactics to manage making up formula in the night i.e. using the ready made stuff.
Mostly I have accepted that two things weighed heavily against me. The tongue tie and my mental health. However when I see information about the benefits of breastfeeding I do get pangs of wishing I had been able to breastfeed and feeling upset I have had to rely on formula. But as a believer that breastfeeding is the default position where possible I think it is fine to continue to share this info widely. Whilst I had pangs about it due to this info, I really think it is so important to promote breastfeeding as the norm. And I feel good knowing that I did my best for me and for baby in the circumstances, and I am proud of a relatively quick recovery from the worst ravages of post partum psychosis. On medical grounds my feeding choice seems to have been necessary, and a healthy mum means a mum who could care for her child. Formula feeding has worked very well for me.
Scott – “I found it very straightforward”

Scott’s wife Charlotte chose to formula feed their son. He doesn’t have any strong feelings about that choice, but he feels that it works for them as “I have been able to help with feeds since he was a very young age.” He doesn’t remember seeing any specific information about infant feeding, but says that he “found it very straightforward”.
Scott’s main concern is about the price of formula milk. “It’s the same price everywhere you shop and for a government obsessed with allowing market forces to dictate every other aspect of our lives, it seems a bit self-contradictory that they should be controlling this in this matter…. especially when some families are working on very tight budgets!”
Lucy – “I love knowing they’re ‘homegrown’ “

“My children have both had breastmilk. I breastfed my eldest exclusively for two weeks, then I switched to formula. I regretted this decision though and started to relactate when he was four weeks old. He was combi-fed for around eight weeks until I established my supply again. He was then breastfed until he was eighteen months, when I decided to wean him. My youngest is unable to breastfeed so I express exclusively for him. It’s very important to me that my children have the milk my body makes specifically for them and their needs.
Support from healthcare professionals has been patchy. Sometimes good, sometimes awful, but mostly just not offered. I met a very good health visitor at clinic with my eldest, who was able to encourage me with relactation, but the others I came across never seemed willing to talk about it – usually I was met with “that’s very difficult.” One health visitor even told me to just stop giving Alfie bottles…. I had no milk at this point, and if I wasn’t in touch with a breastfeeding counsellor then that advice would have ended my attempt to breastfeed there and then. I have found volunteer breastfeeding support workers to be much more supportive and knowledgeable. With Oliver I have accessed the full range, from peer supporters to lactation consultants, and have found the support to be excellent.
With Alfie I had very limited support from friends and family. I hadn’t had chance to make friends with women who had children, so no one understood what relactation actually meant in terms of time and dedication. My husband was the only support I had at that time. He didn’t really understand my drive but he respected my choice and enabled me to do it by simple things like washing up breast pump parts and holding the baby while I expressed. This time round I have lots more support from friends because they have breastfed so they understand. I have had meals brought round for us, offers of babysitting and invitations to friends’ houses for myself and my pump. My husband is more clued up on the importance of breastmilk now too and fully supports my decision to express for Oliver. He does the night feed so I only have to get up to express, and he’s done practical things like buying an in-car power socket so we can still have days out – I pump in the car!
Sadly I don’t have support from other family members. I have been told “I don’t know why you’re faffing with expressing, you’re just being selfish really.” “There’s no need to breastfeed after six months, it’s just wrong and I don’t want to see it.” “Well all mine had formula and they’re okay.”
Most of my infant feeding information comes from International Board Certified Lactation Consultants (IBCLCs) and breastfeeding counsellors. Also from the Kellymom website and other breastfeeding mums.
I feel good about my feeding choice because I know I’m doing the best I possibly can for my boys. I wouldn’t be expressing full time if I didn’t feel the benefits are important. I love knowing they’re ‘homegrown’ “.
*****************************
I asked all of the contributors to read and comment on the Open Letter from the WBTi team, as I feel it is a very important call to action with regards to infant feeding in the UK. This was their responses:
Lucy – “I think the letter is brilliant.”
Liz & Alan – “Good if there is more encouragement and support for breastfeeding. Interesting that more mums are choosing breastfeeding but not sticking at it for very long.”
Sarah-Jane – “I agree with the letter in that mothers are not always given the best chance to breastfeed long term. The hardest time is those first few weeks and if you haven’t got a good support network around you it could be easy to think formula is best or that your baby isn’t getting enough milk from you. The level of support across the country is very much a postcode lottery – if you’re lucky you can get support, if you’re not you’re alone. Not having the support of family can also play a massive part in whether you continue or even consider breastfeeding as an option for your child.
I agree that more needs to be done with regards to the advertising and marketing of formula, including the concept that formula is better or as good as breastmilk. The marketing should be honest and open allowing people the best chance of making the right choice for them. I also agree with the actions of what needs to happen to make the UK a more open, capable, able society for mothers to have the best available information, with the facts, benefits, advantages on each of the feeding choices. It is only then we can be confident as mothers that we can make an informed choice. Support has to be the key: where there is support and peers there is success.”
Lisa – “I agree with the majority of the letter as I still feel now if I was better supported I may have been able to continue breastfeeding.”
Liam – “I agree with all that is said. It takes time to change attitudes and mindsets but it will happen. Perhaps untapped is the father’s input, views and support. Get blokes on side, articulate about breastfeeding, as well as supporting ongoing improvements.”
Sarah – “I think it’s really sad that there is such poor support for something that is so natural. Encouraging support is good, but bombarding women who are probably already struggling with information (which they probably already know) isn’t helpful. That is only my experience of how you’re told breastfeeding is the right thing to do.”
Julie – “I think that the letter should be treated with the importance it deserves and the actions it requests should be given the highest priority by the UK government. I congratulate the contributors. I am continually astonished that more has not been done and more is not done to ensure that breastfeeding rates improve, that the WHO Code is fully acted upon and that there is both training for healthcare professionals and more support for women. It is time now to act and to work together, as a community and as a nation, to improve the health of our babies and of their mothers.”
Laura – “I think it’s an excellent letter and I hope it gets the attention it deserves.”
Scott – “The more education on the subject the better.”
Lucy – “The letter is important, I agree with all of it and I really hope the right people listen and take action.”